 The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. The cookie is used to store the user consent for the cookies in the category "Performance". This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. 
The cookies is used to store the user consent for the cookies in the category "Necessary". The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". The cookie is used to store the user consent for the cookies in the category "Analytics". These cookies ensure basic functionalities and security features of the website, anonymously. Necessary cookies are absolutely essential for the website to function properly. 36 months if the improper payment was due to a recovery by Medicaid, Medicare, the Children’s Health Insurance program or any other state or federal health care program. Print screens are no longer accepted to validate timely filing.Ģ4 months if the improper payment was due to a coordination of benefits error. Medical Claim Dental Claim Vision Claim FSA Claim Short-Term Disability Claim Other Insurance Coverage Request for Predetermination HIPAA Appeals. CLAIMS SUBMITTED WITH DATES OF SERVICE BEYOND 120 DAYS ARE NOT REIMBURSABLE BY CIGNA- HEALTHSPRING. What is the timely filing limit for Cigna?Īs a Cigna-HealthSpring contracted provider, you have agreed to submit all claims within 120 days of the date of service. The two-step process allows for a total of 12 months for timely submission, not 12 months for step one and 12 months for step two. You must submit your claim reconsideration and/or appeal to us within 12 months (or as required by law or your Agreement), from the date of the original EOB or denial. What is the timely filing limit for Cigna claims?Īs a Cigna-HealthSpring contracted provider, you have agreed to submit all claims within 120 days of the date of service. 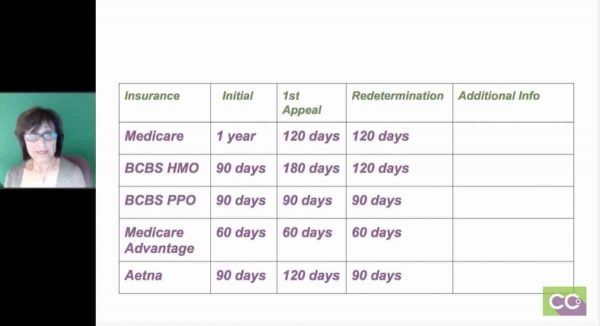
*The timeframe is 180 calendar days for appeals involving utilization review issues or claims issues based on medical necessity or experimental/investigational coverage criteria. What is the timely filing limit for Aetna appeals? 
If you don’t provide this information to us within one year of the date of service, Benefits for that health service will be denied or reduced, as determined by us. It is not based on the date the claim was sent or received. The claims filing deadline is based on the date of service on the claim. You should submit a request for payment of Benefits within 90 days after the date of service. New Jersey - 90 or 180 days if submitted by a New Jersey participating health care provider for a New Jersey line of business member. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
